in Features
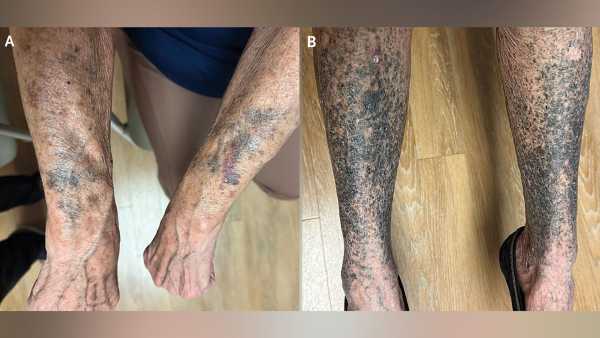
A woman developed striking blue-gray hyperpigmentation on her arms and legs.(Image credit: The New England Journal of Medicine ©2026)Share this article 0Join the conversationFollow usAdd us as a preferred source on GoogleSubscribe to our newsletter
The patient: A 68-year-old female residing in the U.S.
The symptoms: Over a period of six weeks, darkened patches emerged on the woman’s limbs. These splotches varied in hue from a dark blue and purple, resembling bruises, to an intense black.
She also informed her doctors that, two weeks prior to the onset of the patches, she had commenced a regimen of minocycline, an oral antibiotic.
She was prescribed a daily 100-milligram dosage of the medication to address symptoms of rosacea, a condition characterized by chronic facial inflammation and redness. This inflammation can lead to the formation of small, red papules and pustules on the skin, and evidence suggests that antibiotics such as minocycline can help clear these blemishes. Beyond its antibacterial properties, the drug exhibits anti-inflammatory effects, which may offer the best explanation for its efficacy in treating rosacea.
The diagnosis: A recognized adverse effect of minocycline is hyperpigmentation, where areas of skin become darker than the surrounding tissue. In this specific instance, the woman was diagnosed with type II minocycline-induced hyperpigmentation, characterized by “blue-gray discoloration of normal skin on the extensor surfaces of the arms and legs,” as detailed in a report of the case.
The antibiotic can also precipitate two other forms of hyperpigmentation. Type I presents as blue-black discoloration on scarred or inflamed facial skin, as opposed to healthy limb skin, and type III manifests as a muddy-brown pigmentation in sun-exposed regions of the body.
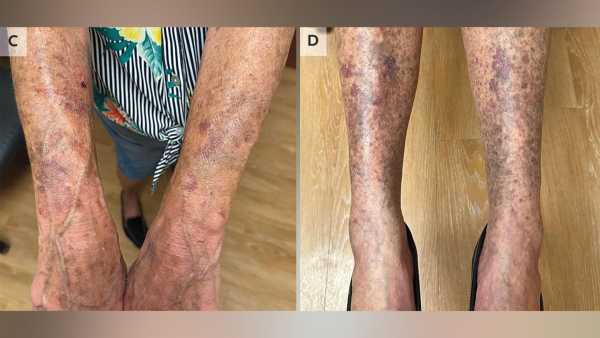
At a six-month follow-up assessment, the woman’s hyperpigmentation had diminished somewhat but remained apparent.
(Image credit: The New England Journal of Medicine ©2026)
The treatment: Medical professionals advised the patient to discontinue minocycline and to limit sun exposure, as ultraviolet radiation is believed to exacerbate hyperpigmentation in such scenarios. Six months later, the hyperpigmentation on her limbs had “somewhat subsided” but was still noticeable.
What makes the case distinctive: Hyperpigmentation is not necessarily an uncommon occurrence for minocycline users with rosacea; one widely referenced study estimates that this side effect affects approximately 28% of individuals in this demographic, although this research involved a limited number of participants. The actual prevalence of the side effect remains uncertain.
This woman’s situation was noteworthy, partly due to the rapid development of the discoloration — appearing within two weeks of initiating minocycline therapy. While type I minocycline-induced hyperpigmentation can emerge shortly after a person begins taking the drug, types II and III typically require a longer interval to become apparent.
“It generally develops after prolonged treatment but can occasionally occur with shorter durations,” the authors of the case report stated. Types II and III are thought to be influenced by dosage, meaning a specific quantity of the drug must accumulate in the body before the dark patches surface.
Other dilemmas
- A toddler accidentally ingested gonorrhea bacteria from a laboratory dish
- Man contracted rabies from an organ transplant after the donor was scratched by a skunk
- A rare semen allergy may have led to a woman’s infertility
The genesis of minocycline-induced hyperpigmentation is not entirely comprehended, but it is theorized to stem from the manner in which the antibiotic is metabolized in the body. The resulting metabolites, or byproducts, bind to iron and are subsequently absorbed by immune cells known as macrophages, where they accumulate. Furthermore, the medication might stimulate the activity of cells responsible for producing melanin—the pigment that imparts color to the skin—while also binding to melanin, thereby forming clusters of dark pigment that persist in the skin.
Once an individual ceases minocycline intake, the pigmentation can take months to years to fade, according to reports. In cases of type III, it may sometimes never fully resolve.
For more fascinating medical scenarios, explore our Diagnostic Dilemma archives.
