There’s yet more evidence that cheap, widely available steroids can help save the lives of critically ill COVID-19 patients. In a new analysis that included data from seven clinical trials, the drugs reduced the risk of death among patients by one-third, compared with patients given only standard care.
Based on the analysis, the World Health Organization (WHO) updated its treatment guidelines for corticosteroids, recommending that those with a severe COVID-19 infection receive the drugs for seven to 10 days as their new standard of care. Those with mild infections shouldn’t get steroids because “current data indicated they would not likely derive benefit and may derive harm” from taking the drugs, the guidelines state.
The new analysis was published Sep. 2 in the Journal of the American Medical Association (JAMA).
Early on, there were hints that steroids could be life-saving for COVID-19 patients. For instance, data from China, published in March in JAMA Internal Medicine, suggested that corticosteroids could reduce deaths among coronavirus patients with “acute respiratory distress syndrome” (ARDS) — a condition where the lungs become severely inflamed and their air sacs fill with pus.
In June, U.K. researchers reported that a steroid called dexamethasone reduced the death rate among COVID-19 patients who required oxygen, either through ventilation or less-invasive methods, Live Science previously reported. But that research had not yet been peer reviewed.
“Without access to full trial details, clinicians were uncertain whether to begin using dexamethasone in patients hospitalized with COVID-19, and if they used it, how they should implement it in practice,” professors of medicine Hallie Prescott and Todd Rice wrote in an editorial about the new analysis, also published today in JAMA.
That said, “there has been widespread adoption of steroids in the care of critically ill patients with COVID-19” since the U.K. report came out, Dr. Nahid Bhadelia, medical director of the Special Pathogens Unit at the Boston University School of Medicine, told Stat News. “This is particularly true in many resource-limited countries where I work,” she noted, given that dexamethasone is cheap and easy to get.
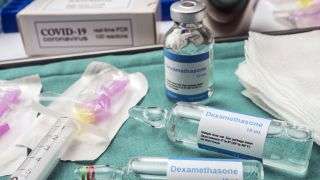
Dexamethasone works by suppressing the immune system and reducing inflammation in the body, and is commonly prescribed for psoriasis, rheumatoid arthritis, asthma and some cancers, such as leukemia, Live Science previously reported. In the new analysis, the researchers looked at trials that tested either dexamethasone or one of two other steroids, hydrocortisone and methylprednisolone. All the drugs similarly dampen the immune response, cause blood vessels to constrict and help to reduce fibrosis, or the development of thick scar tissue, according to the JAMA editorial.
According to the analysis, all three steroids reduced patient mortality at similar rates; overall, the authors calculated a 34% reduction in the risk of death among critically ill patients given steroids compared with those given standard care, Stat News reported. Overall, only 18% of those taking steroids reported serious side effects, compared with 23% of those given standard care; within individual trials, these relative rates differed, but in most of the studies, steroids weren’t associated with a higher risk of side effects.
Related Content
—11 (sometimes) deadly diseases that hopped across species
—14 Coronavirus myths busted by science
—The 12 deadliest viruses on Earth
The new analysis should dispel any remaining doubts about administering steroids to critical COVID-19 patients, Dr. Todd Rice, an associate professor of medicine and critical care physician at Vanderbilt University School of Medicine, told The New York Times. Previous studies of the coronaviruses SARS-CoV and MERS-CoV suggested that steroids might hobble the immune system as it attempts to fight off the pathogens, but that doesn’t seem to be a big concern here, according to the JAMA editorial.
The benefits of steroids outweigh the risks to critical COVID-19 patients, although “the exact threshold at which an individual patient should be prescribed corticosteroids remains unclear,” Prescott and Rice wrote in the editorial. For example, there are different forms of acute respiratory distress syndrome, and steroids may relieve one form of ARDS more effectively than another, they noted. Further research should reveal who exactly should be given steroids, at what dose and when in the course of their illness.
Originally published on Live Science.
Sourse: www.livescience.com





